Benefits of Revision Rhinoplasty: Achieve Your Ideal Nose
Revision Rhinoplasty is a specialized procedure aimed at correcting and refining the results of previous nose surgery. It addresses both aesthetic and functional issues that may have arisen from the initial rhinoplasty, offering a chance to rectify and enhance nasal appearance and breathing functionality. Dr. Bustillo’s expertise in this field ensures that patients receive tailored solutions, focusing on improvement and patient satisfaction.

Dr. Andres Bustillo is an expert in revision rhinoplasty with over 20 years experience and over 4500 nasal surgeries performed to date. Most patients who have revision rhinoplasty with Dr. Bustillo and have realistic expectations end up happy with the results.

What is Revision Rhinoplasty?
Revision rhinoplasty is a facial plastic surgery that involves re-operating on a nose to improve the result of a prior rhinoplasty. This procedure is one of the most difficult plastic surgeries to perform because it is very technically challenging. Damaged soft tissues, fibrosis and scar tissue formation, prior aggressive removal of cartilage and bone can make repair difficult and complex.
Revision rhinoplasty takes two forms. The first is the small “touch-up” revision of an acceptable previous result. The patient may be happy with the overall appearance of the nose but may wish for a slight improvement. The second form is when revision rhinoplasty is performed to transform a previous poor result. Experience, pre-operative planning, and advanced techniques are essential for a good revision rhinoplasty outcome.
According to the American Society of Plastic Surgeons, over 35,000 revision rhinoplasty procedures were performed in the United States in 2022. This number is a 5% increase from 2021 and shows that more people are seeking out this procedure to improve their appearance.

Patient Testimonials: Real Stories, Real Results
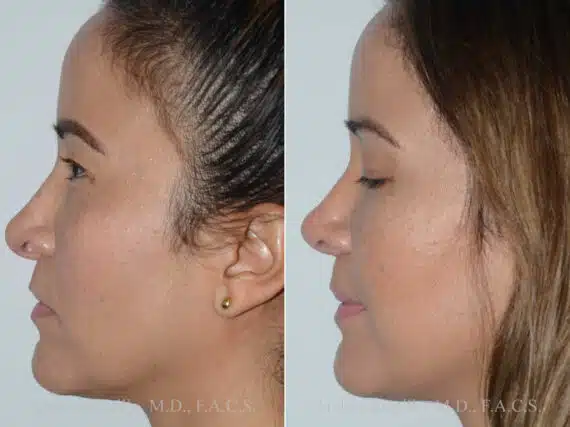
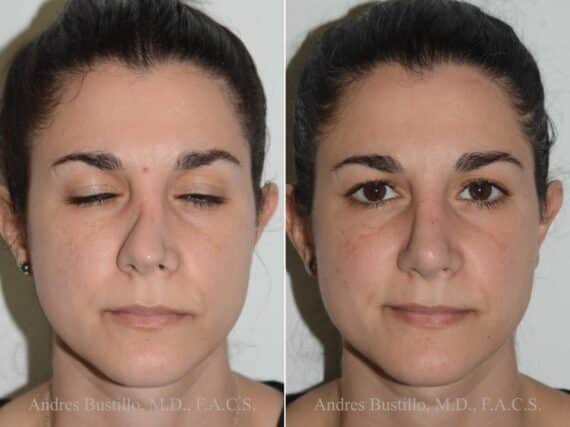
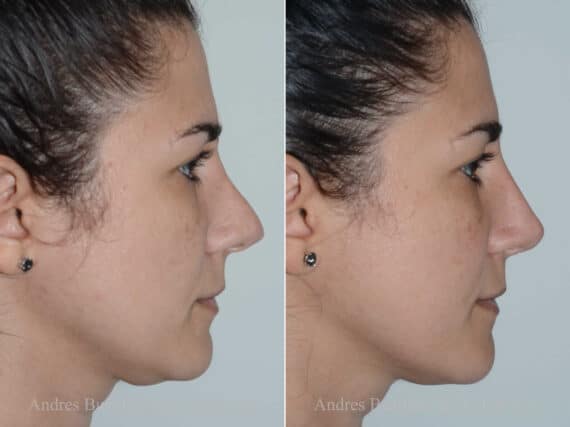
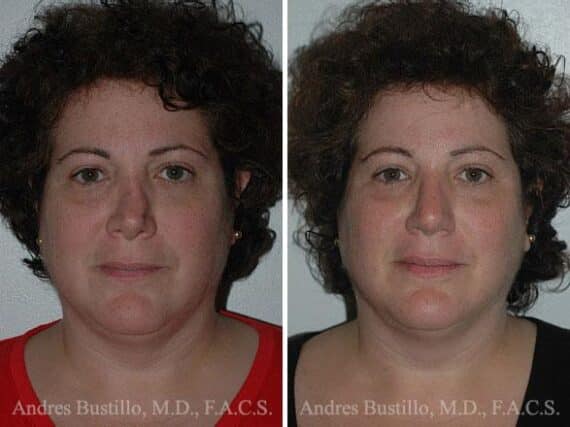
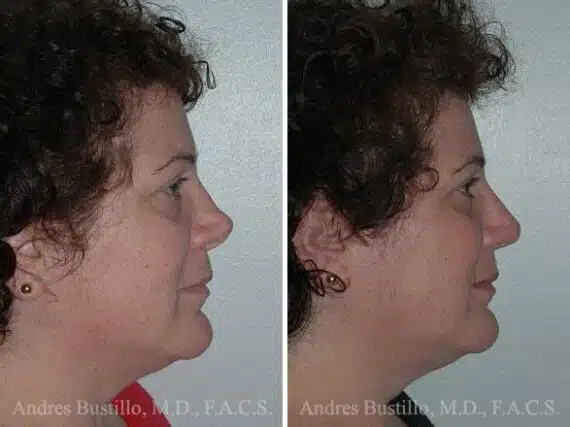
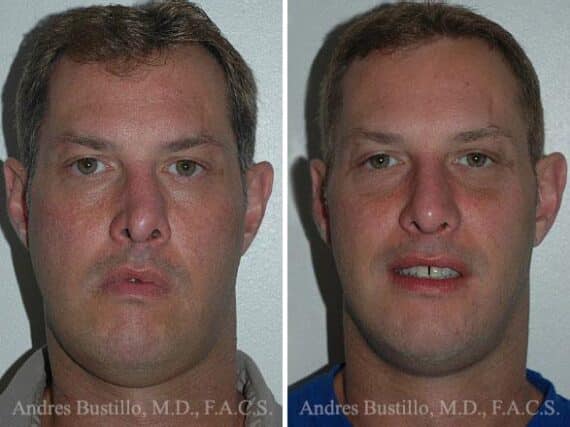
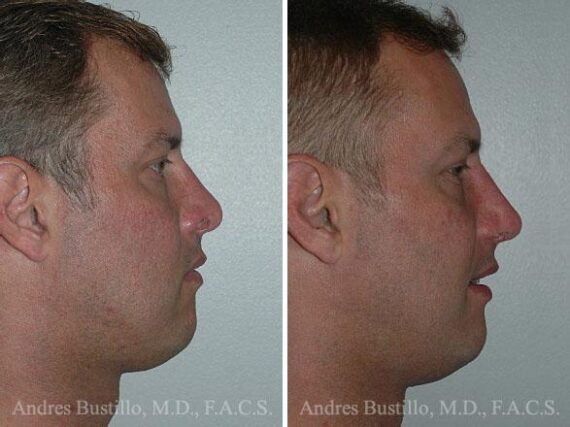
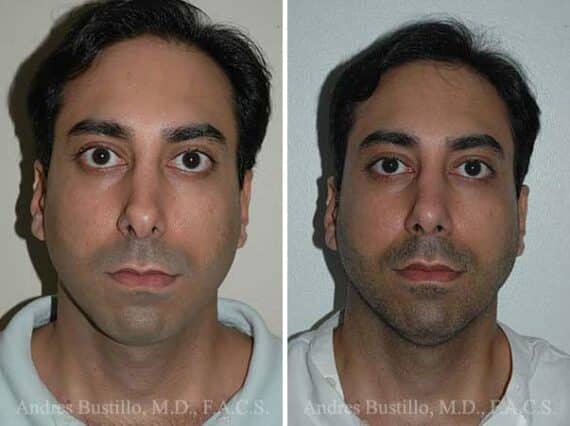
Revision Rhinoplasty Success Stories
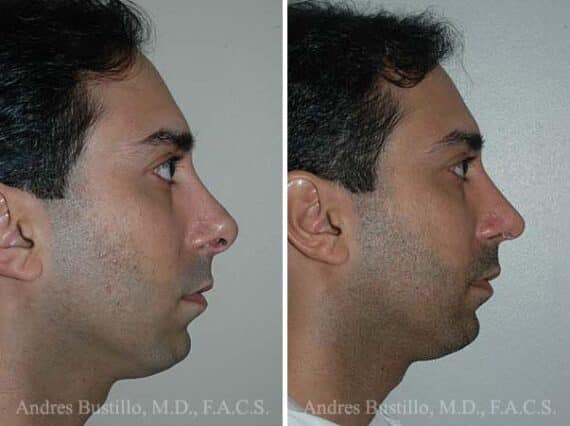
Revision Rhinoplasty Before and After Photos
Each patient is unique and individual results may vary*.
Ideal Candidates for Revision Rhinoplasty
Candidates for revision rhinoplasty in Miami have typically undergone an initial rhinoplasty or more rhinoplasty procedures and are seeking a cosmetic surgeon to address unsatisfactory results.
Most revision rhinoplasty patients are unhappy with the tip, bridge or overall proportion of their nose; they may also have asymmetrical nostrils, have changes to their facial features after trauma, be dealing with severe breathing issues related to a sinus obstruction, or simply want to change the shape of their nose by removing bumps or a hump.
No matter the reason why you think you may need a revision rhinoplasty in Miami, it is best to consult with an experienced cosmetic surgeon who can reassess your specific aesthetic and functional needs. Because some degree of scarring is normal with any rhinoplasty procedure (including revision), careful planning is essential for delivering the most natural-looking results possible.
Questions about your procedure?
Schedule a consultation with Dr. Andres Bustillo.
Consultation for Revision Rhinoplasty
The revision surgery consultation is your opportunity to discuss and address any questions you might have for Dr. Bustillo about revision rhinoplasty and your candidacy.
Dr. Bustillo begins the consultation with a thorough discussion of the concerns you have about the appearance and function of your nose. Next, he will perform a complete physical examination of the inside and outside of your nose, including the status of the septum and the availability of septal cartilage. The amount of tip support and the status of the nasal tip cartilage will be examined.
During the consultation, Dr. Bustillo will also take pictures of your nose. He uses computer imaging as a tool to give patients a clear idea of the possible results of the surgical procedure. He will then explain the procedure and discuss what can be improved and if so to what degree it can be improved.
It is important to provide your surgeon with a detailed medical history of any previous nose surgeries, procedures or treatments. This will help the surgeon to understand the complexity of the revision rhinoplasty procedure and plan accordingly. During the consultation, Dr. Bustillo will also review any previous procedures that have been done on your nose and discuss how they may affect the outcome of your revision rhinoplasty in Miami. He will also take into consideration any medical conditions you may have that could impact your recovery from surgery.

Revision Rhinoplasty Cost
The cost of revision of rhinoplasty depends on the complexity of the procedure and the surgical techniques used. Revision procedures such as revision nose surgery can be more expensive than a primary rhinoplasty due to the additional time and skill required to achieve desired results, typically starting at $19,000. The cost of revision rhinoplasty may also vary depending on the type of anesthesia used and any additional treatments or procedures that may be necessary. Patients should discuss all costs associated with their revision rhinoplasty with their surgeon before undergoing any surgery.
Preparing for Your Revision Rhinoplasty
Before plastic surgery, all patients are required to have pre-operative labs. Patients over 45 or with certain medical conditions are obliged to get medical clearance before their procedure.
Any products that interfere with blood clotting and might worsen bruising should be discontinued ten days before surgery. A full list will be provided for you by our office. Alcohol intake should be stopped five days before surgery to avoid bleeding, bruising, and nasal swelling.
Dr. Bustillo recommends that all patients take 2000mg of vitamin C daily, one week before and two weeks after revision rhinoplasty to improve healing and lessen bruising.

How Revision Rhinoplasty Surgery is Performed
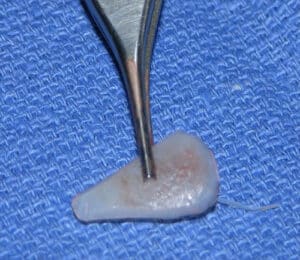
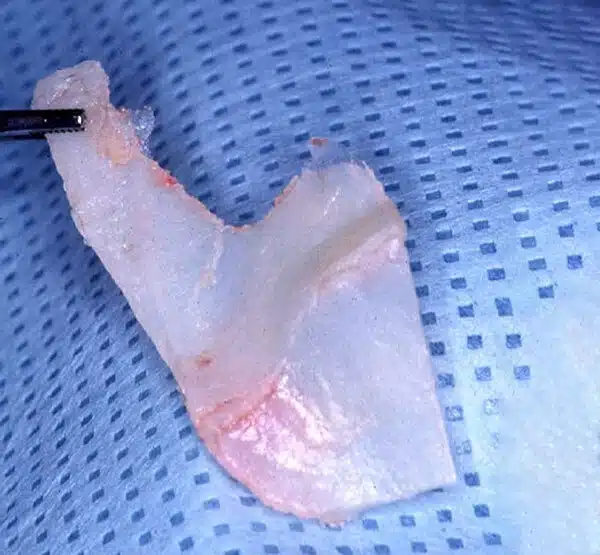
Tip graft used for revision rhinoplasty
Dr. Bustillo performs revision rhinoplasty procedures at his certified surgical facility. The anesthesia is provided by board-certified anesthesiologists (MD) who are part of the Anesthesia Department at Baptist Hospital. Revision rhinoplasty surgery takes between two and four hours to perform using general anesthesia. General anesthesia allows Dr. Bustillo to focus on the revision rhinoplasty surgery while the patient is safely asleep with the airway protected and under the care of an anesthesiologist.
Dr. Bustillo usually performs the secondary rhinoplasty in an open approach. The incision is made in the columella of the nose or the “column” of skin between both nostrils. The incision heals well and will be imperceptible once the patient heals. The open approach allows him to more easily see the areas that are causing deformities in the nose and repair them. Dr. Bustillo will attempt to correct all of the deformities present in the nose, including the bridge, the nasal tip, and the septum.
Recovery Process from Revision Rhinoplasty
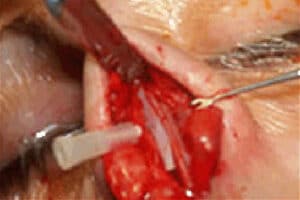
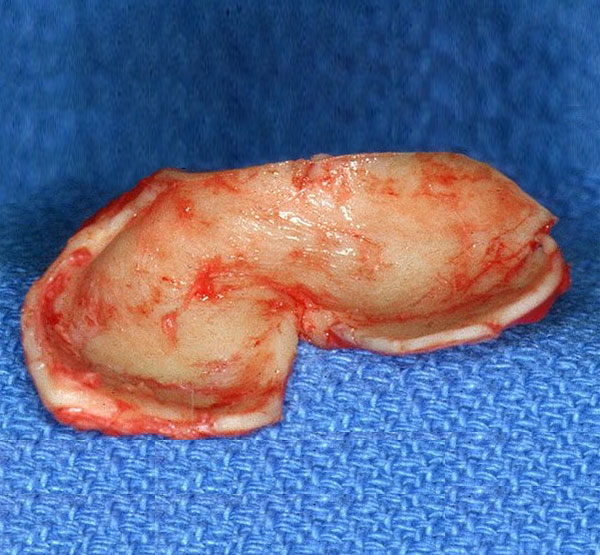
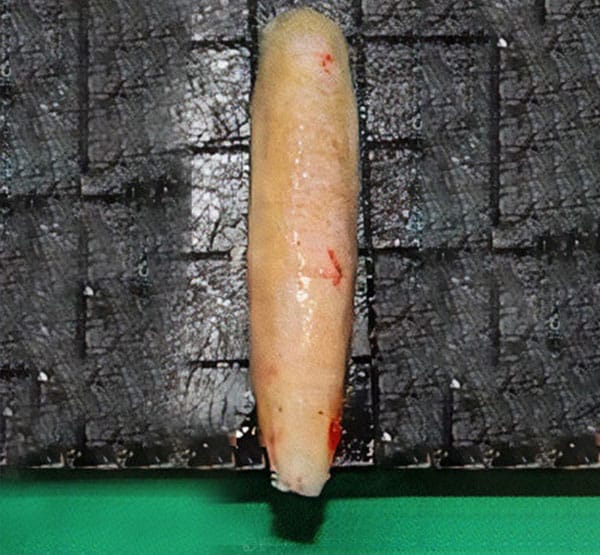
Spreader grafts used for revision rhinoplasty
Patients should plan to spend the night after revision rhinoplasty in a relaxed atmosphere and maintain a liquid diet for twelve hours after anesthesia. Use two pillows at night to keep the head elevated and reduce swelling. Small bags of frozen peas should be kept on the eyes for ten minutes every hour for the first forty-eight hours to reduce eye and nasal swelling. Most patients who undergo revision rhinoplasty experience minimal if any pain. Tylenol is usually enough to control any discomfort.
You will return to the office about 5-6 days after the surgery to remove the nasal cast. The majority of the swelling around the eyes subsides by this time. Most patients can return to work on the sixth postoperative day.
Nasal swelling after a revision rhinoplasty varies. About seventy percent of the swelling resolves after the first month. The remaining thirty percent of the swelling can take from twelve to twenty-four months to completely dissipate. For a smooth recovery from a revision rhinoplasty follow all of Dr. Bustillo’s indications.
After the twelfth month, Dr. Bustillo will take “after” photographs and will give them to you along with the pre-operative photos. The great majority of patients who undergo revision rhinoplasty with Dr. Bustillo are very happy with the final result.

Risks Associated with Revision Rhinoplasty
Candidates for revision rhinoplasty must understand that it is a complex procedure and carries with it specific risks. Anytime a patient chooses to undergo surgery, there will be associated risks that are to be taken into account. When considering revision rhinoplasty in Miami, there are several potential risks of which you should be aware.
The most common risk of revision rhinoplasty is infection or complications from the anesthetic being used. In some cases, your surgeon might choose to use synthetic or artificial materials in order to augment the existing tissue for increased projection and definition. These foreign objects may also present their own set of problems if not correctly placed, such as implant displacement or granuloma formation.
In addition, revision rhinoplasty can lead to prolonged swelling or cosmetic deformities that require further corrective procedures down the line. The shape of your nose may also change over time due to aging, lifestyle habits, and environmental factors, requiring additional surgery in order to maintain your desired look. Additionally, an experienced surgeon often has their own techniques and preferences when it comes to performing a successful revision rhinoplasty — choosing the wrong surgeon could result in subpar results or even damage beyond repair.
Aftercare Following Revision Rhinoplasty
Revision rhinoplasty aftercare is an important part of the recovery process. It is essential to follow your surgeon’s instructions carefully in order to ensure a successful outcome. After surgery, it is important to keep the head elevated and avoid strenuous activity for several weeks. Additionally, patients should avoid blowing their nose or sneezing forcefully as this can cause damage to the nasal septum.
It is also important to be aware of any changes in the appearance of your nose that may occur due to previous surgery or trauma. If you notice any changes, contact your doctor immediately so they can assess the situation and provide appropriate treatment if necessary. In some cases, revision rhinoplasty may be required in order to correct any issues that have arisen from previous surgery or trauma.
In addition, it is important to take care of your nasal septum following revision rhinoplasty. This includes avoiding picking at scabs or crusts that form on the septum and avoiding activities such as swimming or diving which could put pressure on the area and cause further damage. Additionally, using a saline spray regularly can help keep the area clean and reduce inflammation and irritation.
Finally, it is essential to attend all follow-up appointments with your surgeon in order to ensure that the healing process is going as expected.
Revision rhinoplasty in Miami can be a complex and delicate procedure, but with the right surgeon and aftercare, you can achieve the desired results.
Why Choose Dr. Bustillo for Your Revision Rhinoplasty?
Dr. Bustillo is known as a facial aesthetics authority in Miami. He is a double board-certified plastic surgeon with over 20 years in practice and understands how to bring out the best in his patients. He is known for offering natural-looking results from both surgical and non-invasive procedures, prompting his patients to come back again and again.
- Castle Connolly Top Doctor for more than 10 years
- American Board of Facial Plastic and Reconstructive Surgery
- American Board of Otolaryngology-Head and Neck Surgery
- Facial Plastic & Reconstructive Surgery Fellowship at The New York University
- Otolaryngology – Head & Neck Surgery Residency at The University of Miami, Jackson Memorial Hospital
- General Surgery Internship at The University of Miami, Jackson Memorial Hospital