Achieve Facial Harmony with Rhinoplasty
Rhinoplasty is more than just a facial procedure; it’s a life-changing experience that offers a multitude of benefits. From enhancing facial harmony to improving breathing irregularities, this transformative surgery by expert surgeons can significantly boost your confidence and overall well-being.

Patient Testimonials: Real Stories, Real Results

What is the Purpose of Rhinoplasty?
The goal of rhinoplasties performed by Dr. Bustillo is to create a beautiful and balanced nasal structure that fits harmoniously into the rest of the face. By removing the focus from the nostrils and shifting it to the eyes, we achieve a much more pleasing aesthetic outcome. A beautifully proportioned and balanced nasal structure can significantly enhance your overall appearance and self-esteem.
Dr. Andres Bustillo is one of the best nose surgeons in Miami. He is a nose job specialist with extensive experience working with patients of all different ethnic backgrounds, procedures include Caucasian, African American, Asian, Hispanic, and Indian rhinoplasty. With Dr. Bustillo’s expertise and artistry, even minor tweaks to the nose can result in dramatic cosmetic improvements to the entire face.
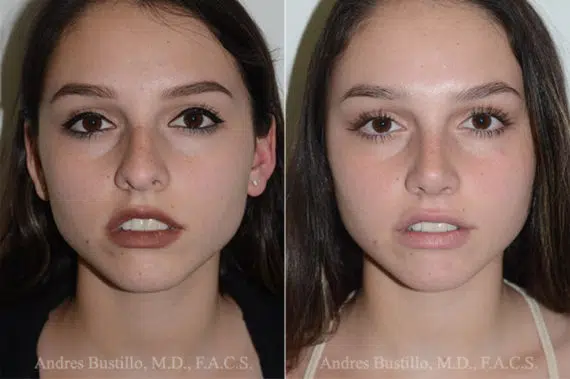
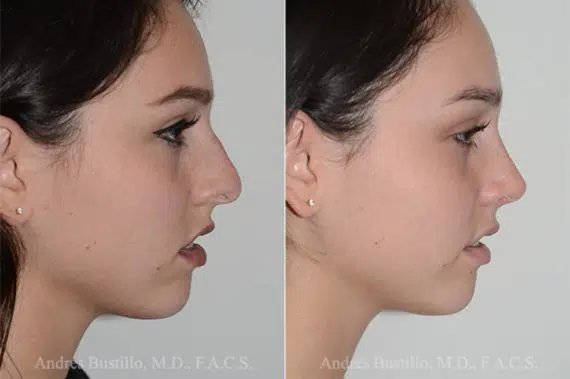
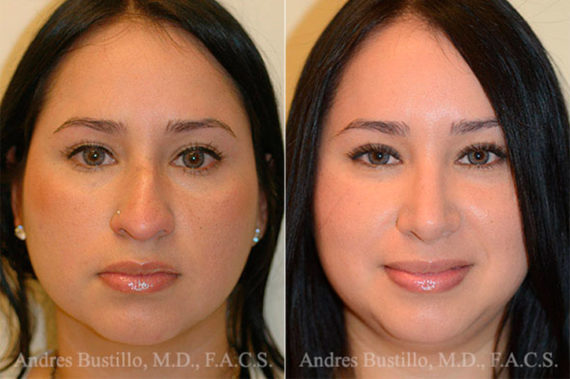
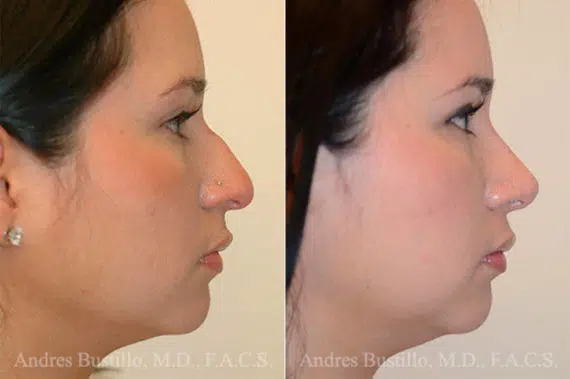
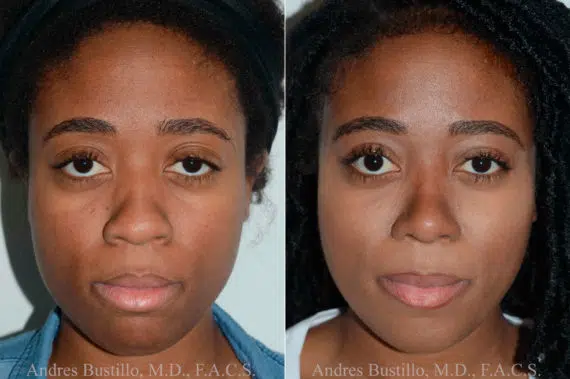
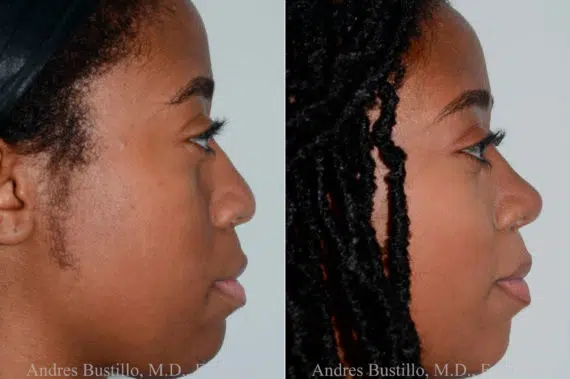
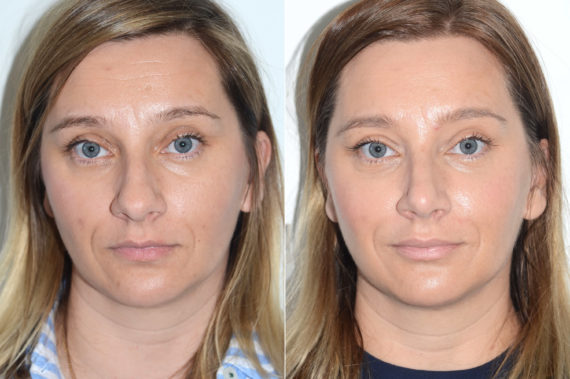
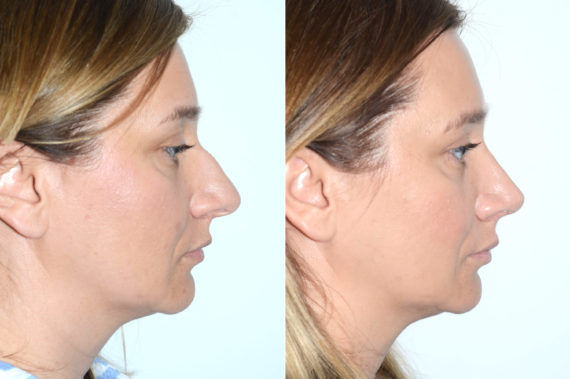
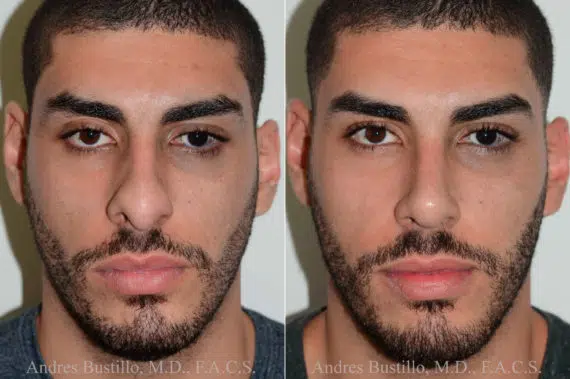
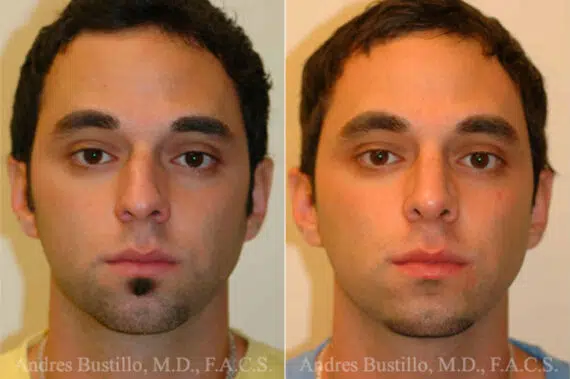
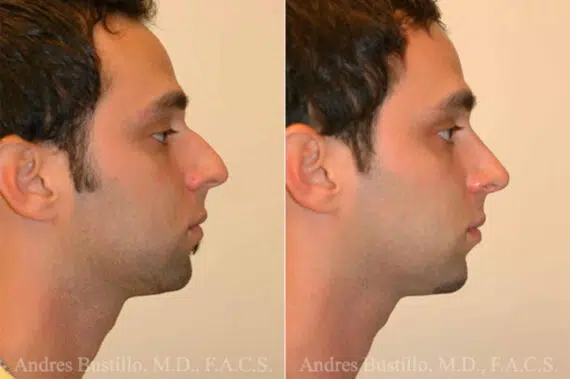
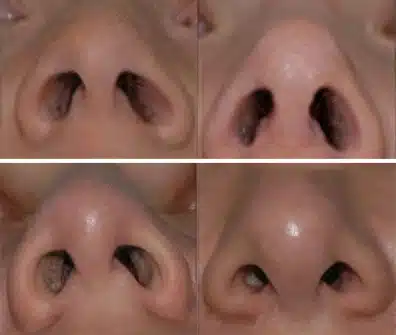
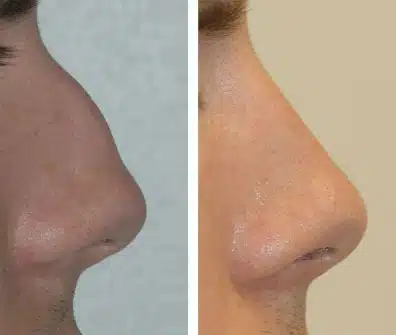
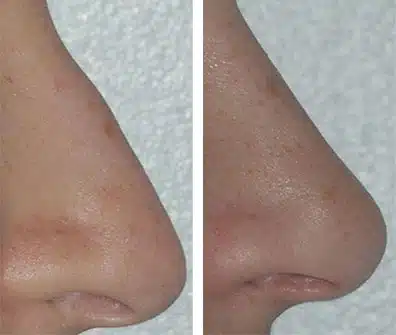
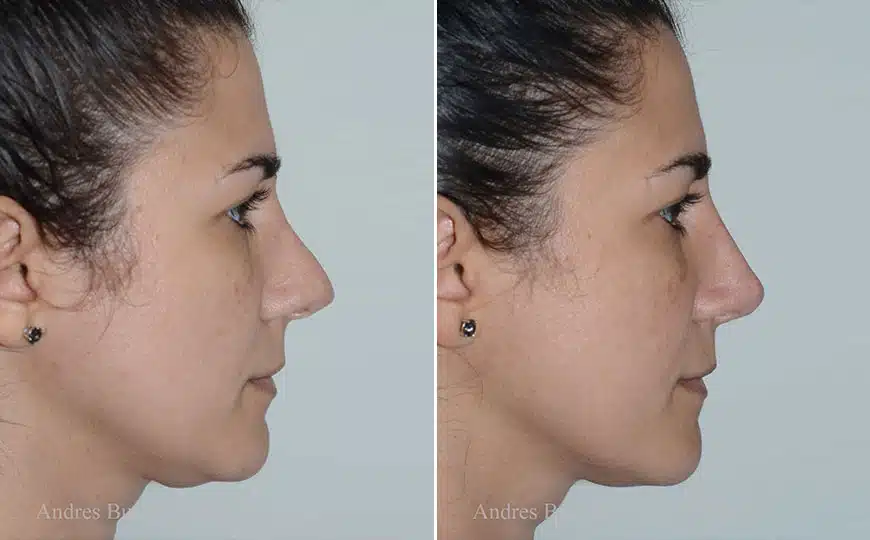
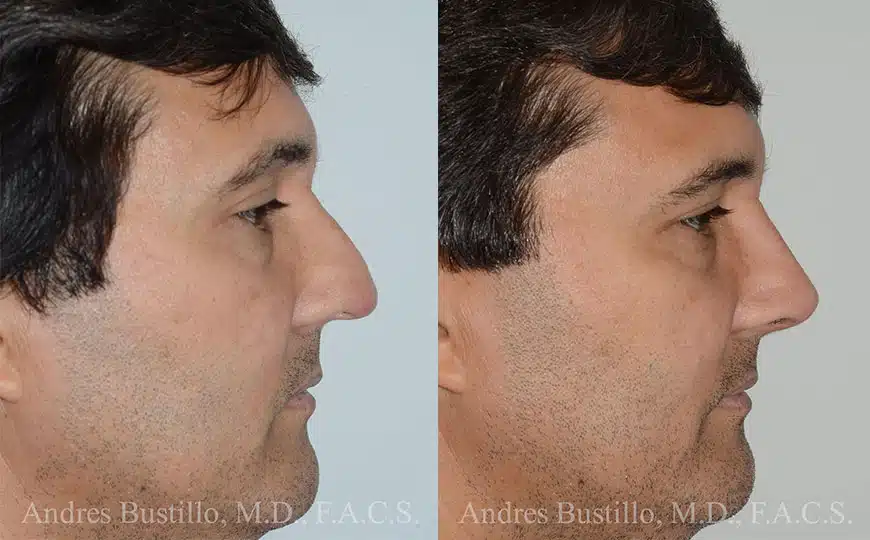
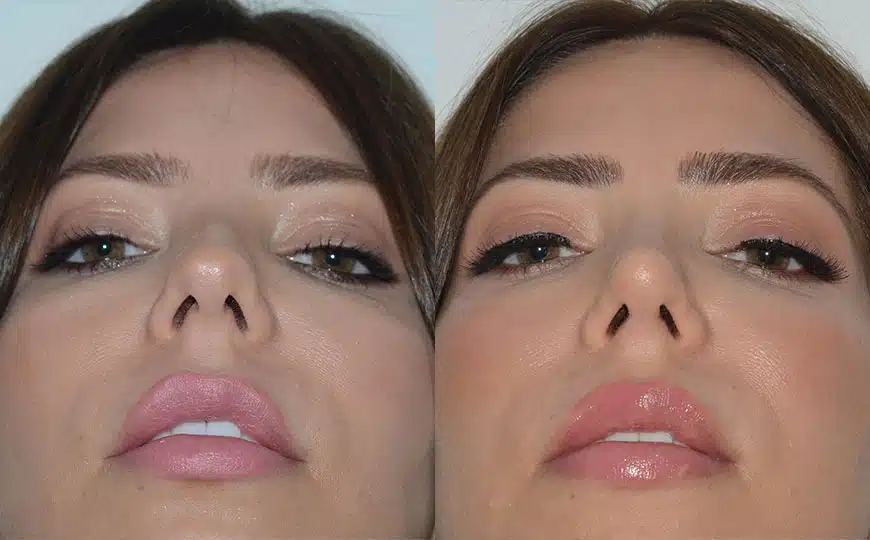
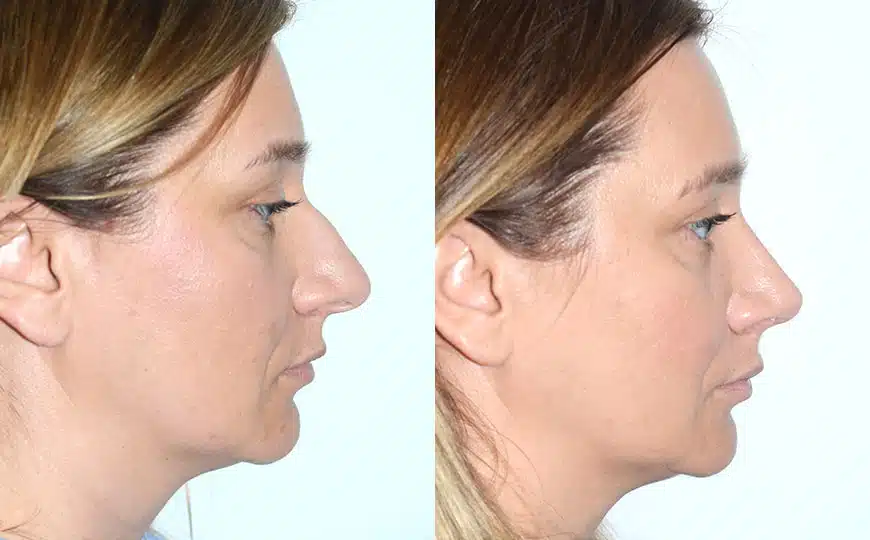
Rhinoplasty Before and After Photos
Each patient is unique and individual results may vary*.
What is Rhinoplasty?
Rhinoplasty, also known as a nose job, is a surgical procedure that changes the appearance of the nose. It’s used to reduce the size of the nose or to narrow the nostrils. Modern rhinoplasty techniques can be categorized into different types, such as Ethnic Rhinoplasty, cosmetic rhinoplasty, and functional rhinoplasty. The surgery is usually done to fix a deviated septal cartilage, remove excess skin, or correct breathing issues. A Primary Rhinoplasty can be performed at any age for rhinoplasty, although most rhinoplasty patients are between 18 and 30 years old. Most patients seek out rhinoplasty as post-traumatic cosmetic surgery after experiencing nasal trauma, such as a Crooked nose, burns, or cuts due to different reasons. Some patients seek out rhinoplasties due to dissatisfaction with their facial shape and bone structure, aiming to achieve their cosmetic goals.

Dr. Bustillo’s personal philosophy regarding rhinoplasty is a fusion of the craft he learned from his mentors and his personal evolution after performing over 4500 nasal surgeries. His philosophy continues to evolve as he serves informed patients and works to provide the best possible rhinoplasty results, whether through Female Rhinoplasty, which often focuses on refining and softening facial features, or Male Rhinoplasty, which typically aims to maintain or enhance masculine facial structure. Each surgical approach, open or closed, is chosen based on the individual’s unique facial characteristics and desired outcomes.
For the last twenty years, there has been a great debate on whether the rhinoplasty operation should be approached in an open or closed fashion. The preferred rhinoplasty method or external incision approach involves an incision in the column between the nostrils.
The closed technique or endonasal approach involves a series of incisions made inside the nose.
One surgical approach is not universally better than the other. Each is used for different types of noses and surgical goals. Dr. Bustillo believes that some noses may be better served with the closed approach and others better treated with the open approach. He uses either approach, depending on the nose.

Questions about your procedure?
Schedule a consultation with Dr. Andres Bustillo.
Dr. Bustillo’s Approach to Rhinoplasty


Why Do People Choose Rhinoplasty?
- Improvement in the size of the nose
- Correct an over-projected tip
- Refined nasal tip
- Correction of weak and droopy tip
- Dorsal hump removal to improve the facial profile
- Enhanced harmony between the facial features
- Improved nasal function and breathing
- Increased confidence and self-esteem
Rhinoplasty Techniques
There are several different rhinoplasty techniques available today. Some surgeons use a combination of these techniques, depending on the patient’s needs.

Structural Rhinoplasty
Dr. Bustillo is an expert in structural rhinoplasty, which is performed by changing the structure of the nasal skeleton using grafts. This is by far the most common type of rhinoplasty performed
Ultrasonic Rhinoplasty
Dr. Bustillo performs all rhinoplasties using the piezo ultrasonic machine, ensuring each procedure is an ultrasonic rhinoplasty. The piezo is used to meticulously reduce the bony portion of the nasal hump and narrow the nasal bones, instead of using traditional rasps. This method is much more precise and limits bruising and swelling post-procedure due to less trauma to the soft tissues.
The piezo ultrasonic machine is also employed to make precise cuts in the bones, replacing the need for osteotomes (chisel and hammer). This technique not only reduces the risk of bruising and swelling but also enhances patient comfort during recovery by ensuring minimal soft tissue trauma. Dr. Bustillo’s utilization of the piezo so consistently across all rhinoplasty surgeries emphasizes his commitment to providing the most advanced and patient-friendly surgical options available.
Preservation Rhinoplasty
Preservation rhinoplasty refers to a series of different techniques with the main goal to preserve the cartilaginous framework of the nose. While Dr. Bustillo has always practiced preservation of the nasal tip cartilages, he now performs dorsal (nasal bridge) preservation in certain cases. This technique minimizes visible scarring and speeds up the healing process.
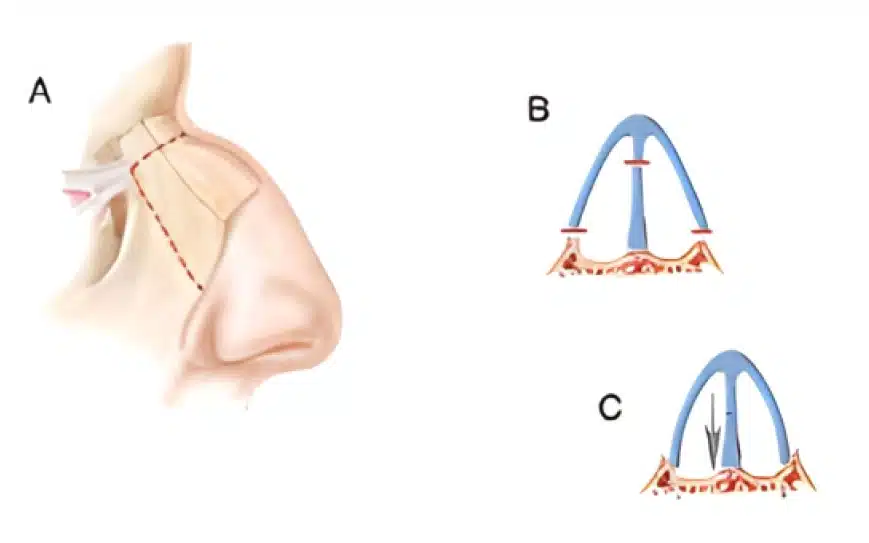
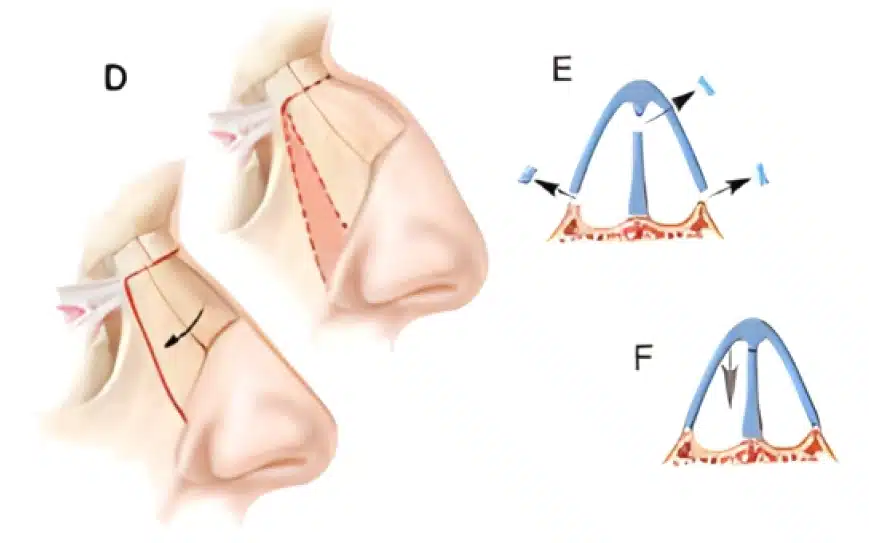
Dorsal preservation involves the reduction of the nasal hump by bringing it down from below instead of removing the cartilage from the top of the hump. Think of reducing the height of the building (the nasal hump) by removing a floor underneath (dorsal preservation) instead of removing the top floor (structural rhinoplasty).
The advantage is that the dorsum or bridge of the nose is preserved and not destroyed. This typically results in a very natural and soft-appearing bridge. The other significant advantage is that one of the preservation techniques available (low septal strip) is the technique that can maximally straighten a deviated nose.
One downside of the dorsal preservation technique is that there is a small percentage of cases where there can be a small 1 mm residual hump. Luckily, this can usually be managed in a small 15-minute retouch done under local anesthesia. The other downside is that there are some patients that may not be candidates for this procedure.
What to Expect During a Rhinoplasty Consultation
Deciding to undergo rhinoplasty is a significant choice. Discuss all options in your initial consultation with your doctor and family before any cosmetic procedure.
- Address concerns about nasal appearance, structural issues like a deviated septum, or breathing problems.
- Includes evaluating medical history to assess surgery risks.
- Essential to have realistic expectations; modern rhinoplasty can improve but not perfect nasal imperfections.
- Dr. Bustillo uses imaging to visualize potential outcomes and align with your goals.
- Comprehensive exam of the external nose, nasal cavities, and septum.
- Assesses nasal hump, bulbous tip, droopy tip, and enlarged turbinates.
- Efficient procedures with minimal downtime, allowing quick return to strenuous activities after the recovery period.
- Positive results, often worth the wait.
By meticulously planning and discussing every aspect of the procedure, Dr. Bustillo ensures that patients are well-informed and prepared for their nose surgery, leading to more satisfactory outcomes and a smoother recovery process.
Who is a Good Candidate for Rhinoplasty?
Whether you are unhappy with the way your nose looks or you face difficulties in breathing due to its structure, this surgery might be suitable for you. It’s designed to correct a variety of issues, from aesthetic dissatisfaction to structural defects that can affect breathing. Below are detailed criteria that help determine if you are a good candidate for nose surgery:
- Ideal if you are bothered by the size or shape of your nose.
- Suitable for individuals looking to alter the appearance of their nasal tip.
- Necessary for those struggling with breathing issues due to nasal structure.
- Recommended for correcting structural irregularities such as:
- A deviated septum — when the cartilage separating your nostrils is off-center.
- Nasal irregularities that impact airflow and aesthetics.
- A broken nose that requires realignment and repair.
- You should be in excellent physical and mental health.
- It’s crucial to not consume alcohol, or be willing to quit prior to surgery.
- Important to have realistic expectations about what rhinoplasty can and cannot achieve.
- Looking for improvement rather than perfection.
- During your consultation, Dr. Bustillo will discuss what the surgery can achieve, set realistic goals, and may also consider chin augmentation to enhance overall appearance.


How Much Does Rhinoplasty Cost with Dr. Bustillo?
When considering a nose job, it is essential to view it as an investment in your self-confidence and well-being. Dr. Bustillo in Miami offers a range of options tailored to your specific needs. While the cost of Rhinoplasty can vary, it typically starts at $17,000, reflecting the expertise and personalized care you’ll receive.
Understanding the Risks of Rhinoplasty
Undergoing nasal surgery involves several risks and considerations that must be thoroughly evaluated with your healthcare professional. Although rare, potential complications can include bleeding, infection, scarring, and more severe outcomes such as nerve damage or even death. Here’s what you need to know before deciding on this surgical procedure:
- Minor complications might include residual swelling and scar tissue formation.
- Serious risks involve bleeding, infection, scarring, and nerve damage.
- In extremely rare cases, complications can be life-threatening.
- Smokers or individuals using illegal drugs are generally advised against undergoing this surgery due to higher risk profiles.
- Discussing all potential risks with your doctor prior to surgery is crucial.
- A common issue post-surgery is the development of a scar tissue lump, often resulting from excessive collagen formation by the body.
- This is particularly noted in cases requiring revision nose job or corrections from previous surgeries.
- It is advisable to consult multiple doctors to thoroughly assess whether nose surgery is the right choice for you.
- Key topics to discuss include each surgeon’s experience, training, and qualifications.
- Understanding the hospital’s policies on insurance and payment plans is also important.
How to Prepare for Your Rhinoplasty Surgery
To prepare for cosmetic nasal surgery, patients should follow these important steps:
- Obtain pre-operative labs as instructed. If over 45 or with specific medical conditions, secure a medical clearance from Dr. Bustillo.
- Cease consumption of blood-thinning products (aspirin, ibuprofen, naproxen) and supplements (vitamin A, Ginkgo Biloba, St. John’s wort) at least 10 days before the surgery.
- Avoid alcohol for five days prior to surgery to reduce potential bleeding and swelling.
- Start a regimen of 2000 mg of vitamin C daily one week before the surgery, continuing for two weeks post-surgery to aid in reducing bleeding and swelling, ensuring a smoother recovery.
How is Nose Job Surgery Performed
Dr. Bustillo performs nasal surgery as an outpatient procedure at his certified surgical facility. Anesthesia is provided by board-certified anesthesiologists (MD), who are part of the Baptist Hospital Anesthesiology Department. The procedure is performed with general anesthesia to help protect the airway during surgery.
Using the latest techniques employed by modern nose job surgeons, Dr. Bustillo will then reshape the nose according to the patient’s specific needs and goals. This could include using the open or closed approach, either using structural techniques or preservation techniques. Dr. Bustillo utilizes the piezo ultrasonic machine in all his surgeries. The procedure usually takes between two to three hours, depending on the complexity and whether it involves external incisions or not.

What to Expect During Rhinoplasty Recovery
Recovery is crucial to the success of your nose surgery and achieving a healthy nasal structure. Follow your surgeon’s instructions closely for optimal healing. Below are some guidelines and aftercare tips:
- Keep your head elevated using two pillows to minimize swelling.
- Apply a cold pack over the eyes for 10 minutes every hour awake during the first 48 hours to reduce swelling.
- Maintain a liquid diet for the first 12 hours post-anesthesia.
- Variable swelling expected; significant reduction typically within four weeks.
- Numbness in the nose tip is common but usually fades within days, though can last weeks.
- Avoid strenuous activities like running or heavy lifting for four weeks.
- Adhere to guidelines about sun exposure and medication usage.
- Remaining swelling may resolve over up to twelve months, revealing the final nose shape.
- Protect your nose from direct sunlight and treat your skin gently.
- Use sunscreen regularly to prevent hyperpigmentation.
- Stay hydrated and eat well to promote healing.
Finding My Perfect Nose
Nina’s Journey: A Rhinoplasty Success Story with Dr. Bustillo
Procedure: Rhinoplasty
Age: 18-year-old
Technique: Open rhinoplasty including septoplasty, hump reduction, caudal septal extension graft, and dome sutures.
Nina chose Dr. Bustillo for rhinoplasty, a decision made with confidence after extensive research. Their consultation set a mutual vision and realistic goals, emphasizing natural results with potential subtle imperfections. On surgery day, Nina’s anxiety was met with compassion and professionalism, ensuring comfort.
The reveal, five days post-operation, was met with positive reactions, even as the expected swelling set in. As her nose gradually took shape over the months, Nina is feeling very content with her new profile and is convinced that her decision to change it has been exceptionally rewarding.
Rhinoplasty Videos

Dr. Andres Bustillo,
MD, FACS
Dr. Andres Bustillo is a renowned nasal surgeon in South Florida, performing over 300 nasal surgeries annually. With over 20 years of experience in facial plastic surgery, he is double board-certified and specializes exclusively in facial procedures, dedicating half of his practice to rhinoplasty and revision rhinoplasty.
Dr. Bustillo is acclaimed for delivering natural and conservative results in rhinoplasty, ensuring the new nose complements the patient’s other facial features and meets functional needs. His expertise extends to various nose types, including ethnic rhinoplasty.
Besides his practice, Dr. Bustillo is an educator, teaching the principles of rhinoplasty to students, residents, and fellow surgeons worldwide, and he is a published author on the subject.
- Best Doctor’s 2020-2021
- Castle Connolly Top Doctor for more than 10 years
- Diplomate American Board of Facial Plastic and Reconstructive Surgery
- Diplomate American Board of Otolaryngology-Head and Neck Surgery
- Facial Plastic & Reconstructive Surgery Fellowship at The New York University
- Otolaryngology-Head & Neck Surgery Residency at The University of Miami, Jackson Memorial Hospital
- General Surgery Internship at The University of Miami, Jackson Memorial Hospital