Rejuvenate Your Look with Facelift Benefits
Miami is a prime spot for facial rejuvenation procedures due to its expert surgeons, aging population, beauty-centric culture, top-notch medical facilities, and perfect recovery environment. The procedure offers a comprehensive solution to the visible signs of aging, creating a refresh and attractive appearance. Some of the benefits are:

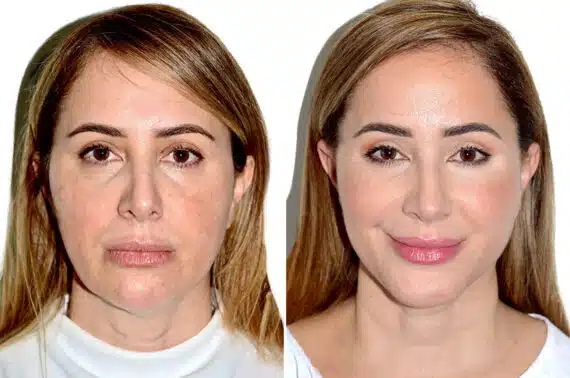
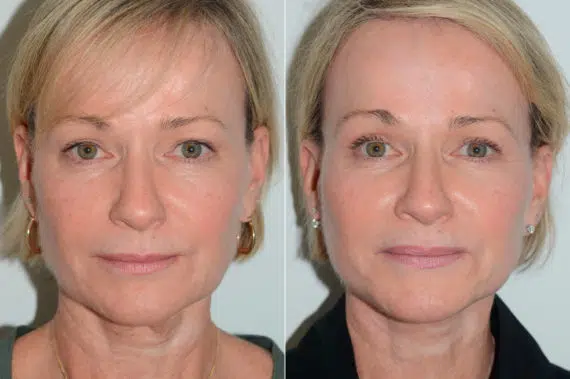
Patient Testimonials: Real Stories, Real Results
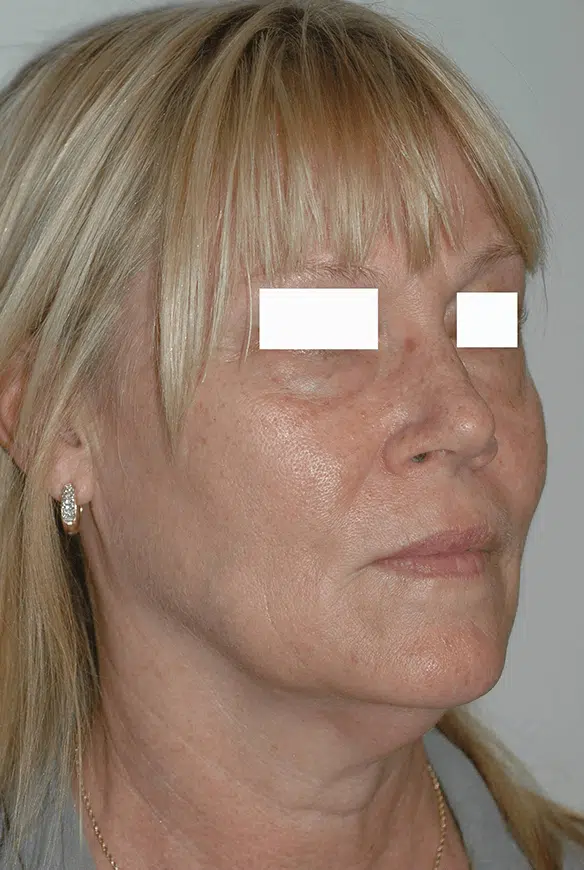
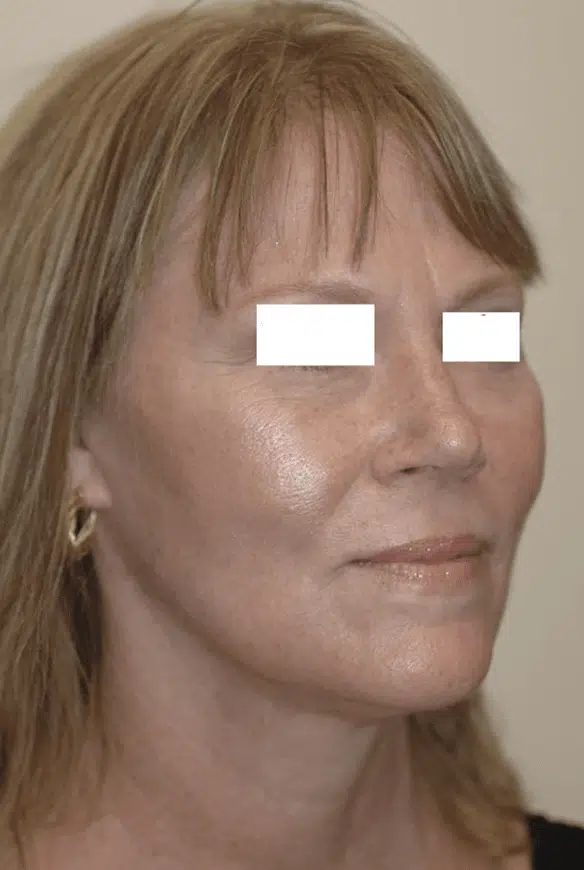
What is a Facelift Procedure?
A facelift procedure is a type of cosmetic surgery that addresses facial aging by:
- Tightening sagging skin
- Reducing deep creases
- Rejuvenating the appearance of the face
Typically performed as an outpatient operation, it involves general anesthesia. This facial plastic surgery, popular among Miami residents for long-lasting results, repositions underlying tissues and removes excess skin to create a more youthful appearance. This procedure effectively enhances the jawline, defines cheekbones, and restores a smoother, more rejuvenated look to the face.
Dr. Andres Bustillo is one of the select facial plastic surgeons with dual board certification. As a facelift specialist focused exclusively on facial cosmetic procedures, he does not perform breast or body surgery and devotes 50% of his practice to facial rejuvenation surgery.
Types of Facelifts
There are different variations of facelift surgery available, each tailored to address specific concerns and goals for surgery. This is why choosing a skilled facelift surgeon is a critical step in your journey towards rejuvenating your appearance. Understanding the different types can help individuals make informed decisions about which procedure is best suited for them.
Surgical Facelift Types
A traditional facelift involves tightening the underlying muscles and removing excess facial skin to smooth out folds and reduce sagging. Subcutaneous tissues are repositioned and sometimes augmented with fillers to enhance the face’s contour and provide a more defined structure.
A deep plane facelift is the gold standard in facial rejuvenation for those seeking long-lasting and more youthful results. This technique involves lifting a connective layer of tissue above the facial muscles, known as the SMAS, to create a tightening effect in the neck, cheeks, and jawline. Dr. Bustillo has been performing this advanced technique for over fifteen years.
A mini facelift is a less invasive surgical procedure that typically addresses the jowls and sagging skin or excess skin on the upper neck. While this procedure is less extensive, it often does not meet patients’ expectations, and many return for a full procedure later on.
Non-surgical Facelift Alternatives
Dermal fillers are used to rejuvenate the face by adding volume to areas that have lost fullness over time. This non-surgical option can help smooth out wrinkles and enhance facial contours, but it does not treat loose skin on the aging neck or heavy jowls. The results are temporary and require periodic maintenance.
Botox injections are another non-surgical alternative that helps reduce the appearance of wrinkles and fine lines by temporarily paralyzing the underlying muscles. While effective for certain facial areas, Botox does not address sagging skin or deeper signs of aging and must be repeated regularly to maintain results.
Non-surgical treatments are also temporary and must be repeated periodically for long-term results. These methods often offer less downtime and can be adjusted to meet individual needs. Plastic surgeons normally recommend a full procedure to reverse the telltale signs of aging.
For those considering different approaches to rejuvenating their appearance, exploring non-surgical alternatives to traditional facelift procedures or mini adjustments can be valuable.
Am I a good candidate for a Facelift?
Facelift plastic surgery aims to rejuvenate facial features and enhance aesthetic appeal, making it a significant consideration for candidates observing signs of aging.
- Ideal candidates are typically between 40 and 60 years old, though healthy individuals older may also benefit.
- It is necessary to have a stable weight before the procedure to ensure lasting results.
- The presence of one or more of the following issues can make you a suitable candidate:
- Sagging skin and muscles from the cheeks to the jawline.
- Loose skin on the neck that might fold.
- Jowls created by sagging tissues along the jawline.
- Loss of muscle tone and excess fat in the face
- Wrinkles and loose skin.
Although a facial enhancement can significantly rejuvenate one’s facial appearance, it does not halt the natural aging process. The effects of the surgery are durable and have almost noticeable scars, with many facelift patients satisfied with their results for years afterward. Consulting with a qualified surgeon is essential to explore suitable surgical options and establish realistic expectations.

Ready to rejuvenate your look?
Schedule a consultation with Dr. Andres Bustillo.
Facelift Surgery Process
A facelift plastic surgery involves several critical steps, each aimed at refining the overall aesthetics and functionality of the skin and facial structure. Dr. Bustillo customizes the facelift procedure for each patient. His signature deep plane facelift lifts the cheek fat back to its natural position and redistributes excess skin without creating a pulled or stretched appearance. Because it targets the deeper muscle layer, the results appear natural and long-lasting.
Preparing for cosmetic facial surgery is an important step that can affect the results of the procedure. Without proper preparation, patients run the risk of increased complications. Dr. Bustillo requires all patients undergoing surgery to pass a comprehensive evaluation before their procedure. This evaluation includes pre-operative labs and medical clearance from their primary care physician.
During their consultation at our Miami clinic, patients undergo a detailed assessment. The consultation will evaluate the elasticity of the skin, the amount of fat and muscle tone, and tissue quality. This ensures that the procedure is tailored to their specific needs for optimal results.
The pre-operative analysis evaluates the quality of the skin, looseness at the jawline, the angle from the chin to the bottom of the neck, and the amount of fat and extra skin present in the neck area. The results are very dependent on the elasticity of the skin. If the skin has had extensive damage, additional procedures may be required.
Patients should stop taking all aspirin, anti-inflammatory products (including naproxen and ibuprofen), and certain vitamins (such as vitamin A, ginkgo biloba, or St. John’s Wort) ten days before the facial reshaping procedure. If you take herbal supplements, check with your plastic surgeon before continuing. Dr. Bustillo recommends that patients start high doses of vitamin C (2000mg/day) one week before and continue for two weeks after facial surgery to help with healing and reduce bruising. Patients should also abstain from alcohol five days before the surgery to minimize swelling and promote healing.
On the day of the surgery, patients should expect the procedure to be performed under general anesthesia to ensure comfort and safety. Dr. Bustillo’s facelift technique involves strategically placed cuts in hidden spots and uses a gentle stitching method to ensure scars are almost invisible, setting him apart from others in his field. This facial plastic surgery is typically performed as an outpatient operation.
Post-operative care involves several important steps, including stitch removal and lifestyle recommendations. Following all post-operative instructions and attending follow-up appointments is essential for the best outcomes.
Facial Procedure Combinations
To address multiple signs of facial aging simultaneously, Dr. Bustillo often combines the facelift procedure with additional complementary procedures like fat transfer for volume restoration or blepharoplasty to rejuvenate the eyelids, or neck lift offering patients a comprehensive facial rejuvenation.
Eyelid surgery, or blepharoplasty, improves the appearance of the upper and/or lower eyelids by removing excess skin and addressing puffiness. This procedure enhances the rejuvenation effect of a facelift, making the eyes look more alert and youthful.
A brow lift raises the eyebrows and smooths forehead wrinkles and frown lines. When combined with a facelift, it provides a harmonious rejuvenation of the upper face, enhancing overall results.
- Neck Lift: Creates a defined jawline and smoother neck contour.
- Fat Transfer: Restores lost volume in the cheeks, under eyes, and around the mouth.
- Chemical Peel: Improves skin texture and tone.
- Chin or Cheekbone Augmentation: Enhances facial contours.
- Rhinoplasty: Refines the shape and size of the nose.
- Lip Augmentation: Adds volume and definition to the lips.

Cost of Facelift Surgery
The cost of facelift surgery can vary widely depending on several factors, including the surgeon’s expertise, the complexity of the procedure, and the specific techniques used. While prices for a facelift typically start at $30,000, additional costs may include anesthesia, surgical facility fees, and any complementary procedures that may enhance the overall results.
Discussing all potential costs during the consultation is essential to understanding the financial commitment involved clearly.
What to Expect During Your Facelift Recovery
Recovery from a Facelift operation involves several important steps and care measures to ensure the best possible outcomes:
Recovery from a facelift operation involves several critical steps and care measures to ensure the best possible outcomes. During the first week, immediate post-procedure care is essential.
Immediate Post-Procedure Care:
- In the hours following the procedure, avoid strenuous activities to reduce swelling and aid recovery.
- Your face will be bandaged initially to protect the skin.
- Pain is usually minimal and manageable with Tylenol. Report any severe pain to Dr. Bustillo immediately, as it could signify complications.
- Dr. Bustillo will check on you the day after surgery to replace the initial bandage with a smaller one for another day.
- Swelling Management: Keep your head elevated using two pillows to help reduce swelling of the face and neck. Place small bags of frozen peas, wrapped in a towel, on the face every fifteen minutes for the first two days to help reduce swelling.
During the second week, the focus shifts to stitch removal and gradual resumption of daily activities.
Stitch Removal and Follow-up:
- Stitches under the chin and in front of the ears are removed five days post-surgery.
- Stitches behind the ears are taken out after ten days.
- Dr. Bustillo will provide additional care instructions for the incision lines.
- Patients can begin to shower and wash their hair five days after surgery.
Weeks three and four are about continuing recovery and gradually returning to normal activities.
Post-Operative Care and Lifestyle:
- Resume strenuous activities three weeks after surgery.
- Return to work approximately two weeks post-surgery.
- Activity Restrictions: Avoid strenuous activities for the first three weeks. Resume light activities as recommended by Dr. Bustillo.
- Makeup Use: Depends on Dr. Bustillo’s advice. Ensure any products used do not irritate the incision areas.
By the end of the first month, most patients see significant improvements and feel more comfortable resuming their daily routines.
Continued Recovery:
- The warm and healing climate of Miami significantly aids in the healing process.
- Full results and recovery from this cosmetic facial surgery may take several months.
- Following all post-operative instructions and attending follow-up appointments is essential for the best outcomes.
- Sun Protection: Avoid direct sun exposure and always use sun protection to help with healing.
- Healthy Lifestyle: Maintain a healthy diet and stay hydrated to promote overall well-being and healing.
Throughout the first year, patients will continue to see improvements and should maintain follow-up visits to ensure optimal results.
Long-Term Care:
- Regular follow-up appointments with Dr. Bustillo to monitor progress.
- Continued adherence to post-operative care instructions to maintain results.


Facelift Potential Risks
While facelift surgery offers transformative results, it is important to be aware of some minor potential risks, which are typically well-managed under professional care. These include:
- Minor Anesthesia Reactions: Complications from anesthesia are rare and usually well-controlled.
- Temporary Numbness: Some temporary numbness in treated areas may occur but typically resolves on its own.
- Mild Swelling and Bruising: Swelling and bruising are common but generally subside within a few weeks.
- Minimal Scarring: Scarring is refined and usually well-hidden, with proper post-operative care enhancing healing.
- Rare Infections: Infections are rare and can be effectively treated if they occur.
- Temporary Adjustments in Facial Nerves: Minor and temporary adjustments in facial nerve function are possible but usually resolve quickly.
Choosing Dr. Andress Bustillo, an experienced and board-certified surgeon, ensures that these minor risks are minimized, allowing for a safe and precise procedure.
Feeling Youthful Again with Dr. Bustillo
Real Patients’ Story
Procedure: Facelift
Age: 40s
Technique: Standard facelift
After noticing loose skin around her neck, the decision to undergo a facelift became clear. Extensive research led to the choice of Dr. Bustillo for his renowned care. The pre-operative experience was marked by a reassuring call from Dr. Bustillo, ensuring a calm and confident approach to the surgery.
The post-operative period was notably smooth, with minimal discomfort experienced only on the first night. By the second week, recovery was nearly complete. The professionalism and attentiveness of the staff at Dr. Bustillo’s office further enhanced the experience, leaving her feeling naturally refreshed and profoundly satisfied with the results. Her gratitude towards Dr. Bustillo’s expertise is immense, and she highly recommends his services.
Procedure: Facelift
Age: 61
Technique: Natural and imperceptible incisions
After noticing her neck getting worse over several years, Livia began considering plastic surgery. Though she had always believed in “aging gracefully,” her neck’s condition prompted a serious re-evaluation. A close friend referred her to Dr. Bustillo, and after several consultations, Livia knew he was the right choice. His excellent bedside manner, soft-spoken nature, and honesty stood out. Dr. Bustillo thoroughly explained the aging process and what results Livia could realistically expect, providing a clear and reassuring picture.
The night before the surgery, Dr. Bustillo’s comforting call eased Livia’s nerves. On the morning of the surgery, the anesthesiologists and nurse provided additional reassurance. Dr. Bustillo marked her face and prepared her for surgery. The first night post-surgery was uncomfortable but not painful. The next day, Dr. Bustillo removed the bandage, revealing an amazing new neck, though her cheeks were still swollen. Dr. Bustillo reassured her that the swelling was normal, a fact she remembered reading in the provided manual. Over the next two weeks, the swelling subsided, and Livia began to see the full results. She felt rejuvenated and happy, looking like herself but more rested and well. Friends complimented her improved appearance without realizing she had surgery. Livia’s confidence soared, and she would gladly undergo the procedure again, only with Dr. Bustillo.
Procedure: Deep plane facelift, upper and lower eyelid surgery, and fat transfer
Age: 68
Technique: Comprehensive facial rejuvenation
Despite believing in aging gracefully, Norma, a 68-year-old woman with an active social life, felt her facial appearance didn’t match how she felt inside. Feeling increasingly self-conscious, she discussed facial rejuvenation surgery with her initially hesitant family. Recalling a friend’s praise for Dr. Andres Bustillo, Norma decided to seek a consultation. Impressed by Dr. Bustillo’s thorough explanation of age-related facial changes and his conservative, natural approach, she felt confident and supported, especially when her family warmed to the idea. Norma opted for Dr. Bustillo’s recommendation: a deep plane facelift, upper and lower eyelid surgery, and fat transfer.
A calming call from Dr. Bustillo the night before the surgery reassured her. On the surgery day, the staff’s professionalism, including Dennise’s comforting care and a reassuring anesthesiologist, put her at ease. Post-surgery, Norma experienced only minor discomfort. Dr. Bustillo’s follow-up care, including removing her bandage and addressing her concerns about swelling, helped her through the recovery. By the second week, Norma saw significant improvements and received compliments on her refreshed look without anyone guessing she had surgery. Her hairdresser even praised the fine, barely visible incisions. Reflecting on the journey, Norma is immensely grateful for Dr. Bustillo’s expertise and wishes she had undergone the procedure earlier. She highly recommends his services.

Why Choose Facelift Surgeon Dr. Andres Bustillo?
Dr. Bustillo is known for his dedication to plastic surgery and also known as a facial aesthetics authority in Miami. He is a double board-certified plastic surgeon with over 20 years in practice and understands how to bring out the best in his patients.
Dr. Bustillo regularly teaches students, residents, and other physicians in facial rejuvenation surgery. He has shared his advanced facelift techniques with plastic surgeons in South America, Asia, and the Caribbean, cementing his international reputation.
Dr. Bustillo is an experienced surgeon who is known for offering natural-looking results from both surgical and non-invasive procedures, prompting his patients to come back again and again.
- Best Doctor’s 2020-2021
- Castle Connolly Top Doctor for more than 10 years
- Diplomate American Board of Facial Plastic and Reconstructive Surgery
- Diplomate American Board of Otolaryngology-Head and Neck Surgery
- Facial Plastic & Reconstructive Surgery Fellowship at The New York University
- Otolaryngology-Head & Neck Surgery Residency at The University of Miami, Jackson Memorial Hospital
- General Surgery Internship at The University of Miami, Jackson Memorial Hospital